What you want to know (in less than one minute):
- The gut doesn’t just digest food — it contains millions of nerves and bacteria that communicate with and influence the brain due to a phenomenon known as the “gut-brain connection”
- Science now shows a connection between mental health disorders, substance use disorder and gut health; some research even suggests that an unhealthy gut may increase the risk of relapse after recovery
- Many factors can lead to an unhealthy gut — but there are ways to restore balance and diversity to your gut flora and increase your overall well-being
Curious yet? It’s time to dig into the eye-opening science behind mental health, substance use disorder and gut health.
What is The Gut-Brain Connection?
The “gut” includes not only your entire digestive tract but also the roughly 100 trillion bacteria living inside it. Most of us understand that the gut plays an important role in digesting food and absorbing nutrients. But science shows there is a connection between the brain and the gut, as well.
For over 25 years, people from all over the world have chosen Waismann Method as their opioid detox provider.
We know the challenges you face and the importance of creating a unique and personal experience for you right from the start.Call for Detox Options 1-800-423-2482
This connection is so important that the gut has a nickname: the “second brain,” or enteric nervous system (ENS). Here’s why:
In addition to bacteria, the gut is home to roughly 200 to 600 million neurons—that’s about the same number of neurons found inside the spinal cord. These neurons are similar in size and function to the brain and play a role in a number of important processes, including:
- Mood, including anxiety and depression
- Emotions
- Learning and memory
- Inflammation
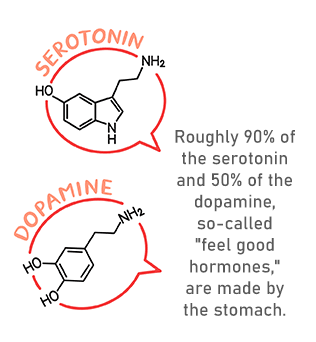
The gut communicates with the brain via parasympathetic fibers of the vagus nerve (the word “parasympathetic” describes the part of the nervous system involved in rest, relaxation, and digestion). This two-way connection between the brain and the gut is known as the gut-brain axis, and helps explain the phenomenon of feeling physical symptoms of anxiety or other powerful emotions, such as “gut feelings” or “butterflies in the stomach.”
Thanks to the ongoing communication between the gut and brain, any factors that negatively affect gut health can ultimately affect mental health — and may play a role in an individual’s susceptibility to substance abuse disorder, anxiety, depression, and related conditions.
Gut Bacteria and Addiction
Numerous studies reveal a link between substance abuse and the gut.
As just one example, one study published in PNAS found that people with abnormal amounts of gut bacteria had higher rates of anxiety, depression, and cravings for alcohol after nearly three weeks of treatment for alcohol addiction. In comparison, individuals with healthier guts fared better. The differences were so significant that the researchers hypothesized poor gut health was associated with an increased likelihood of relapse.
It’s worth nothing that the link between substance use disorder and the gut goes both ways. Gut bacteria are capable of influencing addiction-related mechanisms like motivation, stress, and reward, whereas substance use itself can cause abnormal changes in the gut flora. These changes may further drive addiction-related behaviors and increase the likelihood of subsequent health complications, such as colon cancer in the case of long-term alcohol use disorder.
How the Gut-Brain Connection Influences Mental Health Disorders
Many people are familiar with stomach problems associated with anxiety, depression, and related mental health conditions. These problems include diarrhea, nausea, constipation, or even the sensation of having a “pit in your stomach.”
We now know that these physical symptoms are normal consequences of abnormal gut function characterized by an imbalanced gut microbiome, or the community of bacteria found inside the gastrointestinal (GI) tract.
How does this bacterial imbalance develop? Researchers know that stress, inflammation, and other factors promote the growth of harmful bacteria inside the digestive system, which can crowd out “friendly” bacteria and damage the delicate gut lining, contributing to so-called leaky gut syndrome. When the gut lining is inflamed and damaged, partially digested food, toxins, and other waste products are able to seep into the body where they can spread and irritate other tissues and organs, including the brain.
These harmful bacteria also interact with gut fibers, and—thanks to the gut-brain axis—can influence the number and type of neurotransmitters and hormones released by the brain. These neurochemical changes can ultimately contribute to unhealthy behaviors like overeating and substance use, which only further drives the cycle of mental illness and gut dysfunction.
There is also evidence to support a protective relationship between mental health conditions like depression and the gut. A 2016 study from Science discovered that people with depression tend to lack certain species of gut bacteria, suggesting that a properly functioning and diverse gut environment can support or perhaps improve mental and emotional well-being.
In other words: it’s not just genes, history of trauma, and physical or emotional distress that can influence the development of mental health issues. The health, biodiversity, and overall function of a person’s gut can also influence a person’s risk of anxiety, depression, and other mood disorders.
So, What Now? How to Improve Gut-Brain Function
Improving your gut health is an important step in boosting your mood and may even help lower your risk of mental health issues and substance use disorders. Maximizing your gut health can also help drive recovery from these common health concerns and enhance your long-term outcomes—a good gut may even help reduce the risk of relapse.
Thankfully, improving gut health is largely within your control.
Here are a few areas to focus on:
- Diet: when you eat, you’re not just feeding yourself—you’re also feeding the bacteria inside your gut. And it turns out that “friendly” bacteria and “bad” bacteria prefer different things. To maximize gut health, make the bulk of your diet come from whole and minimally processed foods, including healthy fats, quality protein, vegetables, and fruits. Fruits and veggies
in particular are rich in fiber which healthy bacteria thrive on. Nutrient dense foods also contain the vitamins, minerals, and antioxidants your gut and brain need for optimal function. In the meantime, avoid processed foods and refined sugar, which can promote inflammation and feed the harmful bacteria.
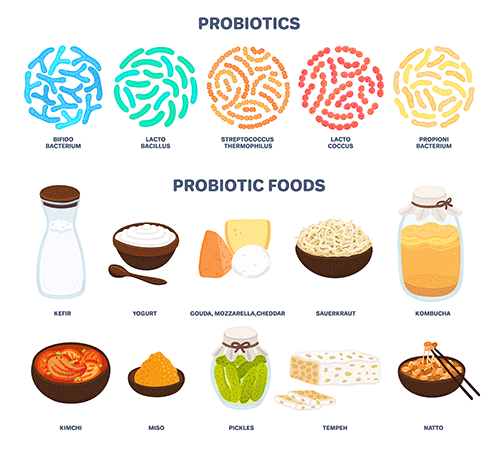
- Supplements: supplements can’t replace a healthy diet. But they can enhance the beneficial impact of the foods you’re eating and an overall healthy lifestyle. Talk to your doctor about whether you should introduce certain supplements into your routine, including multivitamins, omega-3 fatty acids, and probiotics (including strands of good bacteria like bifidobacterium and lactobacillus). You can also experiment with adding fermented foods to your diet, such as apple cider vinegar, kefir, and sauerkraut, which help introduce healthy bacteria into your digestive system.
- Stress management: a dysfunctional gut can increase levels of stress-related hormones in the body, which can drive inflammation when they stay elevated for too long. Poorly managed stress can also drive unhealthy habits like overeating and substance use. So, learning how to manage your stress appropriately has a huge impact on your overall health and your recovery journey. Practice strategies like meditation, exercise, deep breathing, progressive muscle relaxation, and other techniques to keep yourself calm.
- Psychotherapy: interventions such as cognitive behavioral therapy (CBT) may enhance communication between the gut and the brain and therefore may help reduce physical symptoms associated with anxiety and the gut.
Conclusion
The link between mental health, substance use disorder and GI dysfunction is strong—and it goes both ways. When the gut is unhealthy, it can negatively influence brain function, impair mood, and drive addiction-related behaviors. Mood disorders and substance abuse disorders can further contribute to the growth and development of harmful bacteria.
The good news is that your gut health is largely within your control. There are simple steps you can take, with the help of your provider and medical team, to heal your gut, heal your brain, and change the direction of your life.
Sources:
- Harvard Health Publishing: Can Gut Bacteria Improve Your Health?
- NCBI: Gut Feelings: The Emerging Biology of Gut–brain Communication
- PNAS: The Gut Microbiota as an Environmental Factor That Regulates Fat Storage
- NIH: The Role of the Gut Microbiome in Opioid Use
- NCBI: Colorectal Cancer and Alcohol Consumption – Populations to Molecules
- NCBI: Stress, Depression, Diet, and the Gut Microbiota: Human–Bacteria Interactions at the Core of Psychoneuroimmunology and Nutrition
- Science: Population-Level Analysis of Gut Microbiome Variation
- John Hopkins Medicine: The Brain-Gut Connection
Written by Sara McEvoy, PT, DPT
Sara is a licensed and board-certified Doctor of Physical Therapy. She earned her undergraduate and graduate degrees from Boston University. Sara is also a professional freelance writer and copywriter. She researches and writes primarily within the health and wellness fields.
Reviewed by Clare Waismann, Registered Addiction Specialist (RAS), Substance Use Disorder Certified Counselor (SUDCC), founder of Waismann Method® Advanced Treatment for Opiate Dependence and Domus Retreat®. Clare Waismann is an authority and expert on opioid dependence, opioid use disorder, substance dependence, detoxification treatments, detox recovery, and other topics covered on RapidDetox.com.

 in particular are rich in fiber which healthy bacteria thrive on. Nutrient dense foods also contain the vitamins, minerals, and antioxidants your gut and brain need for optimal function. In the meantime, avoid processed foods and refined sugar, which can promote inflammation and feed the harmful bacteria.
in particular are rich in fiber which healthy bacteria thrive on. Nutrient dense foods also contain the vitamins, minerals, and antioxidants your gut and brain need for optimal function. In the meantime, avoid processed foods and refined sugar, which can promote inflammation and feed the harmful bacteria.




